Most people eat for different goals without realising they’re undermining every single one of them. The runner training for a marathon uses the same nutritional approach as their mate, focusing on muscle gain.
The person chasing fat loss mirrors the diet of someone reversing sarcopenia (age-related muscle loss). Same meals, same timing, same macronutrient (protein, carbohydrate, fat) ratios. Different objectives, identical strategy.
This doesn’t work because your body responds to nutrition based on what you’re asking it to do. Research demonstrates that elite athletes and recreational exercisers require fundamentally different nutritional approaches, even within the same sport.
Fat loss demands a negative energy balance; muscle gain requires a surplus. Cognitive performance responds differently to macronutrient composition than to physical endurance.
Throughout this piece, you’ll find evidence on fat loss through caloric manipulation, muscle gain via protein timing, performance nutrition for strength versus endurance, metabolic (energy-processing) health through micronutrient (vitamins and minerals) balance, and strategies for healthy ageing, bone health, and cognitive function.
Some sections include interactive tools that let you explore the data yourself rather than passively reading numbers. No lectures on what you should do. Just the mechanisms, the evidence, and the applications.
Your goal dictates your fuel. Everything else is noise.
The Foundation: Why You Must Eat for Different Goals
Your body doesn’t interpret a calorie deficit as “fat loss mode.” It interprets scarcity. Protein surplus doesn’t automatically translate to muscle gain. It means amino acids (protein building blocks) require metabolic processing. The outcome depends entirely on the physiological demand you’ve created.
When you train for strength, your muscle fibres develop microtears that require repair via muscle protein synthesis (the muscle-building process). A daily protein intake of 1.6 to 1.7 grams per kilogram of body mass supports this adaptation. Endurance athletes, conversely, need 1.2 to 1.4 grams per kilogram.
Their metabolic priority shifts toward restoring glycogen (stored carbohydrate) and maintaining sustained energy availability. Same nutrient, different requirement, dictated by the adaptive stress placed on tissues.
Nutritional requirements aren’t fixed characteristics. They’re responses to total energy intake, carbohydrate availability, exercise intensity and type, training history, age, sex, and even the timing of nutrient intake. A 30-year-old gaining muscle requires different strategies than a 70-year-old preventing sarcopenia, despite both focusing on lean mass.
Research on older adults shows that protein intake exceeding 20 grams per day becomes necessary to stimulate muscle protein synthesis. A threshold that doesn’t apply uniformly across age groups.
Individual variation compounds this complexity. The RISSCI-1 study tracked responses to dietary fat modification and found changes in LDL cholesterol (harmful cholesterol type) ranging from -38% to +19% among participants following identical protocols. Genetic makeup, gut microbiome (digestive bacteria ecosystem) composition, metabolic health status, and lifestyle factors all influence how your body processes the same meal.
Personalised nutrition approaches have demonstrated superior outcomes compared to generic dietary advice. With significantly greater reductions in saturated fat intake, processed meat consumption, and improvements in overall diet quality.
The point: when you eat for different goals, you’re not following arbitrary rules. You’re aligning nutrient intake with physiological demands your body cannot meet through willpower or training intensity alone.
Fat Loss Through Nutrition: Creating Your Deficit
Fat loss requires one rule: consume fewer calories than you burn.
The non-negotiables:
- Weight loss rate: 0.5-1 kg per week preserves muscle
- Protein: 1.6-2.2 g/kg daily protects lean tissue during restriction
- Carbohydrate: minimum 3-4 g/kg maintains training intensity
- Fat: typically 0.7-1.3 g/kg, adjusted to create the deficit
These aren’t suggestions. They’re evidence-based boundaries separating effective fat loss from metabolic slowdown.
The calculator above lets you adjust protein, carbohydrate, and fat intake. Watch which fat loss strategies your ratios support. Move the sliders to see real-time compatibility with continuous restriction, intermittent fasting, time-restricted eating, low-carbohydrate approaches, and exercise-based protocols.
Timing strategies that work:
Time-restricted eating (6-8 hour feeding windows) produces superior fat mass reduction compared with unrestricted eating. Intermittent fasting shows measurable outcomes: body weight down by 2.05 kg, BMI reduced by 0.73 kg/m², fat mass decreased by 2.14 kg whilst preserving lean tissue.
These aren’t magic. They’re structured approaches making adherence easier for specific individuals.
Individual responses vary wildly. Some thrive on intermittent fasting. Others perform better with consistent meal timing. Stress, sleep quality, training volume, and baseline metabolic (energy-processing) health determine which approach, when you eat for different goals like fat loss, actually works beyond theory.
The deficit creates the outcome. The method determines whether you sustain it.
Muscle Gain: The Protein and Timing Equation
Protein builds muscle. Everyone knows this. Few understand that the equation has three variables, not one.
1: Amount matters: 1.6 to 2.2 grams per kilogram body weight daily optimises muscle protein synthesis (building process) during resistance training. Higher intakes (3.2 g/kg) don’t provide additional benefits for most parameters except peak power.
2: Timing matters: Muscle protein synthesis operates in windows. Post-exercise represents peak sensitivity. Before bed supports overnight repair. Spreading intake across multiple meals maintains elevated synthesis rates compared with infrequent, large doses.
3: Context matters: A 30-year-old male gaining muscle requires different strategies than a 16-year-old adolescent or a 50-year-old woman. Adolescents show 18% greater whole-body protein assimilation capacity when normalised to fat-free mass. Women in the luteal phase (the second half of the menstrual cycle) have higher protein requirements due to increased tissue turnover.
The tool above builds your evidence-based protocol. Select your age, sex, training focus, and experience level. It reveals personalised protein targets, timing strategies, creatine dosing, caloric surplus recommendations, and the research supporting each variable.
Creatine enhances the equation. Supplementation with 3 to 5 grams daily increases muscle creatine stores, supporting adaptations to high-intensity training. Heavier individuals may require 5-10 g daily to maintain optimal stores. When you eat for different goals like muscle gain, creatine represents one of the few supplements with consistent evidence across populations.
Energy Surplus Fuels Adaptation
Muscle growth requires raw materials and metabolic capacity. Adequate caloric intake (approximately 29 kcal/kg/day) supports significant muscle hypertrophy during training. Positive energy balance alleviates energetic stress that interferes with anabolic (building) adaptations.
The slower the weight gain, the higher the proportion of muscle versus fat. Rapid gains typically include more water and adipose (fat) tissue. Progressive approaches prioritising weekly gains of 0.25-0.5 kg optimise body composition outcomes over time.
Combine these elements. Daily protein exceeding 1.6 g/kg, distributed strategically, supported by creatine, fueled by caloric surplus. The equation solves itself when variables align.
Athletic Performance: How to Eat for Different Goals in Sport
Sport type dictates fuel strategy. A marathoner and a powerlifter both train hard. Their nutritional requirements sit at opposite ends of the spectrum.
Endurance demands carbohydrate dominance:
- Daily intake: 6-10 g/kg maintains glycogen (stored carbohydrate energy) stores
- Protein: 1.2-1.4 g/kg supports repair and maintains lean mass
- Fat: secondary energy source during prolonged, moderate-intensity efforts
Strength and power prioritise protein and timing:
- Daily intake: 1.6-1.7 g/kg optimises muscle protein synthesis (building process)
- Carbohydrate: sufficient levels (5-8 g/kg) replenish muscle glycogen post-training
- Timing: pre-workout carbohydrate, post-workout protein window critical for adaptation
The profiler above reveals evidence-based nutrition for your sport. Select endurance, strength, power, or team sports. Compare macronutrient (protein, carbohydrate, fat) targets, timing protocols, supplement priorities, and hydration strategies backed by research.
Elite and recreational athletes require different approaches, even within the same sport. Elite footballers with optimised energy metabolism utilise supplements like caffeine, melatonin, magnesium, and creatine chelate more effectively than non-elite players. Recreational athletes respond better to beta-alanine and carbohydrate-protein combinations.
When you eat for different goals across sport types, supplement selection shifts dramatically. Endurance athletes benefit from nitrate supplementation for oxygen efficiency. Strength athletes respond to creatine supplementation by increasing phosphocreatine (a quick energy compound) stores. Team sport athletes require both, timed strategically around match demands.
Training volume and intensity modify these baselines. High-intensity, high-volume periods demand increased carbohydrate to prevent glycogen depletion. Tapering phases allow a gradual reduction while maintaining protein intake to preserve muscle. Periodisation extends beyond training into nutrition strategy.
Your sport determines your fuel. Everything else adjusts accordingly.

Healthy Ageing: Nutrition for Muscle Preservation
Between the ages of 60 and 70, sarcopenia (age-related muscle loss) affects 5 to 13% of people. Over 80, which jumps to 11-50%. The decline isn’t inevitable. It’s nutritionally modifiable.
Muscle protein synthesis operates differently in older adults. The threshold shifts. Where younger individuals respond to modest protein doses, older adults require exceeding 20 grams per meal to trigger synthesis. Below that threshold, dietary protein fails to effectively stimulate muscle maintenance. This isn’t a preference. It’s physiology.
The Health ABC study tracked older adults and found that higher protein intake reduced lean muscle mass loss over time. Not maintained it. Reduced the rate of decline. Adequate protein becomes protective, slowing what otherwise accelerates.
Specialised oral supplements show promise beyond standard protein. Research tested formulations rich in whey and casein proteins, branched-chain amino acids (protein building blocks), vitamin D, and ursolic acid (plant compound) in calorie-restricted mice experiencing muscle atrophy (breakdown).
The supplement attenuated catabolic (breakdown) pathways and supported anabolic (building) signalling. Human trials with branched-chain amino acids plus 12 weeks of progressive resistance exercise improved physical performance in older adults by enhancing mitochondrial (cellular energy) function.
Resistance training remains non-negotiable. Protein without mechanical stimulus provides raw material with nowhere to go. Combined, they prevent muscle mass loss during energy restriction, potentially increasing resting metabolic rate and improving long-term weight maintenance.
Sarcopenic obesity presents a compounded challenge. Prevalence increases with age: 4.2% in those aged 70 to 79.9 years, jumping to 12.2% in those aged 80 to 89.9 years. When you eat for different goals, such as simultaneous fat loss and muscle preservation in older adults, protein requirements rise further while total calories drop. The margin for error narrows considerably.
Micronutrient co-ingestion matters. Vitamin D, B vitamins, and minerals alongside protein may further support muscle protein synthesis. Single-nutrient focus misses the mechanistic complexity. Ageing demands a multifaceted nutritional strategy, not isolated interventions.
The window for intervention opens early. “Possible sarcopenia” can be identified through low muscle strength or low physical performance in primary care settings. Early lifestyle changes, particularly protein optimisation and resistance training, offer protection before clinical sarcopenia manifests.
Muscle preservation in ageing isn’t about reversing time. It’s about reducing the velocity of decline through strategic nutrition meeting altered physiological thresholds.
Metabolic Health: Balancing Blood Sugar and Lipids
Your calcium-to-magnesium ratio predicts mortality risk more reliably than either mineral alone.
Ratios above 3.5 or below 1.7 independently increase cardiovascular disease, cancer, metabolic syndrome, type 2 diabetes, and all-cause mortality. The optimal range is 2.0 to 3.5. Most people have no idea where they fall.
Macronutrient priority creates metabolic trade-offs:
High-fat patterns → increased motivation, reduced cognitive flexibility
High-carbohydrate patterns → initial cognitive advantage, opposite motivational effect
Protein emphasis → improved glucose metabolism in diabetics, enhanced satiety (feeling full and satisfied after eating)
You cannot optimise everything simultaneously. Prioritising one outcome compromises another.
The ranker above visualises these trade-offs. Drag macronutrients into priority order. Watch motivation, cognitive performance, glucose response, and lipid (fat-like substance) profiles shift in real-time. No single arrangement optimises all four. When you eat for different metabolic health goals, understanding these interactions helps you determine your strategy.
Vitamin D function depends on calcium-to-magnesium balance. The vitamin D receptor operates optimally at ratios around 2.0. Magnesium acts as a cofactor for enzymes that convert vitamin D into calcitriol (active form). Without adequate magnesium, vitamin D activation fails regardless of supplementation dose.
Higher calcium-to-magnesium ratios may require elevated vitamin D concentrations to achieve biological activity. This mimics pseudo-vitamin D resistance. Addressing the mineral imbalance proves more effective than increasing vitamin D alone.
Magnesium deficiency links to multiple conditions:
- Arrhythmias (irregular heartbeat) and heart failure
- Type 2 diabetes and insulin resistance
- Alzheimer’s disease progression
- Migraine frequency and severity
Standard serum (the liquid part of blood) testing misses deficiencies because it poorly reflects total body stores. Dietary assessment combined with ratio calculation provides a better indication.
High-protein diets positively affect calcium absorption and bone turnover. But protein without magnesium creates an imbalance. The synergy between nutrients matters more than individual intake levels.
Simple lifestyle modifications effectively prevent or delay metabolic complications. Exercise with proper mineral balance and macronutrient distribution creates outcomes that medication cannot replicate. The combination proves more potent than either intervention alone.
Metabolic health isn’t about hitting isolated targets. It’s about understanding nutrient interactions, accepting trade-offs, and selecting priorities aligned with your specific goals.
Healthy Weight Gain: When More Is the Objective
Gaining weight is harder than losing it. Not physiologically. Psychologically.
The goal isn’t more mass. It’s more muscle. The distinction determines everything.
The Arithmetic
300 to 500 calories above maintenance = approximately 0.45 kilograms per week
Six eating occasions daily versus three = better muscle-to-fat ratio
Slower progression = higher quality gain
The timeline above shows a 12-week progression under different strategies. Select meal frequency (3 vs 6 daily), caloric surplus (+200, +300, +500), and protein distribution. Watch muscle gain accumulate alongside fat gain. The slower approaches produce superior body composition outcomes.
Meal frequency matters beyond total calories. When you eat for different goals like healthy weight gain, distributing intake across six occasions (three main meals plus three snacks) supports muscle protein synthesis better than cramming calories into fewer meals.
Effective snack options:
- Yoghurt with granola
- Peanut butter and jelly sandwiches
- Cereal with whole milk
- Fruit smoothies with protein powder
- Turkey sandwiches on wholegrain bread
These aren’t random choices. They combine protein, carbohydrates, and digestibility.
Resistance training remains non-negotiable. Surplus calories without mechanical stimulus become adipose tissue (fat storage), not contractile tissue. The body responds to demand. Create demand through progressive overload. Supply raw materials through a consistent surplus. Simple equation, difficult execution.
Time becomes the variable most people underestimate. Rapid weight gain feels productive. Numbers on scales climb. But composition suffers. Research confirms slower rates favour muscle over fat and water accumulation.
Energy balance governs outcomes. When intake matches expenditure, weight stabilises. To gain, intake must exceed expenditure consistently, not sporadically. Weekend binges don’t compensate for weekday deficits. The body averages poorly across time.
Patience produces better results than aggression. A 200-calorie daily surplus over 12 weeks beats a 500-calorie surplus over 6 weeks for muscle-to-fat ratio, even when total weight gained appears similar.
The objective isn’t scale movement. It’s tissue quality.
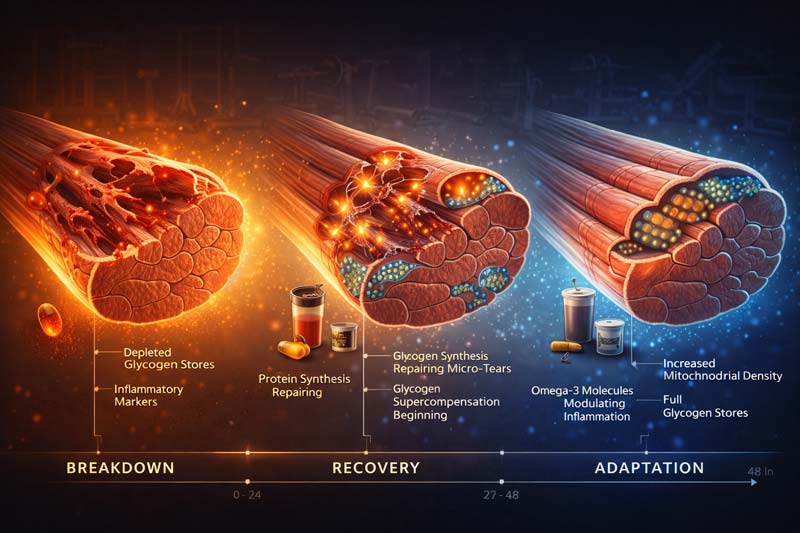
Recovery and Adaptation: Supporting Your Training
Training breaks you down. Recovery builds you back up.
The confusion lies in thinking workouts create strength. They don’t. They create damage. Micro-tears in muscle fibres, depleted energy stores, and elevated inflammatory markers. You finish weaker than you started.
Adaptation happens between sessions when nutrition meets tissue damage. Protein synthesis is activated. Glycogen supercompensates (muscles store extra glycogen after depletion). Mitochondrial density increases (relating to a cell’s energy producers). The body doesn’t just repair. It overcompensates.
What Actually Drives Recovery
Omega-3 fatty acids alter inflammation at the cellular level. They integrate into immune cell membranes, changing how cells respond to training stress. Research shows that 4 grams of EPA and DHA (omega-3 fats found mainly in oily fish) daily significantly reduces inflammatory cytokine (inflammatory signalling molecule) production whilst preserving adaptive signals.
Not eliminating inflammation. Modulating it. There’s a difference.
Post-exercise protein timing exploits windows of heightened muscle sensitivity:
- Immediate post-training: peak synthesis rates
- 24-48 hours: elevated sensitivity continues
- Threshold: 20-25 grams per meal for most adults
- Older adults: higher thresholds required
Below threshold, synthesis plateaus regardless of total daily intake.
Sport Type Determines Recovery Fuel
Endurance athletes recovering from glycogen depletion:
- Carbohydrate: 6-10 g/kg daily concentrated post-exercise
- Timing: within 30 minutes maximises glucose transport
- Protein: 1.2-1.4 g/kg supports muscle maintenance
Strength athletes repairing tissue damage:
- Protein: 1.6-1.7 g/kg distributed across the day
- Carbohydrate: 5-8 g/kg replenishes muscle glycogen
- Creatine: 3-5 g daily supports phosphocreatine restoration
The macronutrient (protein, carbohydrate, fat) priority flips depending on primary training stress.
The Adaptation Paradox
Energy restriction during heavy training blocks adapts. Caloric deficit signals scarcity. The body prioritises survival over building capacity. Muscle protein synthesis drops. Recovery slows. Performance stagnates.
Adequate energy intake (approximately 29 kcal/kg daily) removes this brake. Research confirms that significant muscle hypertrophy only occurs when energetic stress doesn’t interfere with anabolic (building) signalling.
When you eat for different goals involving performance progression, maintaining energy balance during high-volume phases becomes non-negotiable.
Individual Recovery Variation
Some athletes thrive on back-to-back training. Others need extended recovery between sessions. Genetic factors, training age, sleep quality, and baseline inflammation levels all modify recovery capacity.
Omega-3 status correlates with strength and power in young adults. Those with higher EPA levels demonstrate superior recovery markers and performance outcomes. Supplementation can’t override poor sleep or chronic stress, but it addresses one modifiable variable.
Branched-chain amino acids (protein building blocks) combined with resistance training improve physical performance in older adults by enhancing mitochondrial (cellular energy) function. The combination matters more than either intervention alone.
Timing Beyond the Workout
Pre-sleep protein supports overnight repair. Casein protein (slow-digesting milk protein) provides sustained amino acid release during the 8-hour fasting period. Research shows 30-40 grams before bed increases muscle protein synthesis rates throughout sleep without disrupting rest quality.
This doesn’t replace post-workout nutrition. It extends the recovery window, maximising total daily synthesis.
Recovery Determines Progression
Training creates stimulus. Nutrition permits response. Without adequate recovery support, increased training volume produces fatigue accumulation, not adaptation.
The deficit between damage and repair determines whether you progress or plateau. Close the gap with strategic nutrient timing, adequate energy availability, and an appropriate macronutrient distribution to meet your training demands.
Bone Health: The Overlooked Protein Connection
Calcium dominates bone health advice. Supplement aisles dedicate entire sections to it. Doctors test for it. Nutritionists prescribe it.
Protein gets ignored.
Yet epidemiologic studies consistently show protein intake correlates more strongly with bone mineral density than calcium supplementation alone. Higher protein intake is associated with a reduced risk of hip fractures in postmenopausal women. Not marginally. Significantly.
The mechanism isn’t mysterious. Protein directly affects calcium absorption and bone turnover. Increased protein intake raises circulating parathyroid hormone (a hormone that controls blood calcium) concentrations, which enhances calcium absorption efficiency in the gut. More dietary protein means better calcium utilisation, not worse.
The Bone-Protein Evidence
High protein intake doesn’t leach calcium from bones. It strengthens them:
- Inhibits age-related bone loss
- Decreases osteoporosis-related fracture risk
- Increases bone mineral density across populations
- Improves bone homeostasis (internal stability) when combined with adequate minerals
This contradicts decades of calcium-only messaging. The body requires structural material to build bone matrix. Protein provides it.
When Balance Breaks
Protein alone isn’t sufficient. The mineral balance determines whether dietary protein supports or undermines bone health.
Magnesium matters critically. Without adequate magnesium, vitamin D cannot activate properly. The vitamin D receptor functions optimally at a calcium-to-magnesium ratio of around 2.0. Higher ratios create pseudo-vitamin D resistance, mimicking deficiency despite supplementation.
Vitamin K2 enters this equation too. Sufficient K2 mitigates calcium-magnesium imbalances, directing calcium into bone tissue rather than soft tissues, where it causes arterial calcification.
High protein without these minerals creates problems. High protein, combined with balanced minerals, supports skeletal strength.
Who Benefits Most
Overweight individuals, elderly populations, and anyone at fracture risk. These groups show the most significant benefit from protein optimisation for bone health.
The prevalence of overweight and obesity exceeds 60% in developed nations. Global ageing accelerates. Both conditions compromise bone integrity through different mechanisms. Adequate protein consumption becomes a protective intervention, not an optional enhancement.
When you eat for different goals, including bone preservation, protein requirements may reach 1.2 to 2.0 grams per kilogram daily, depending on age, sex, and metabolic health status.
Practical Reality
Most bone health interventions focus exclusively on calcium and vitamin D. They miss half the equation.
Protein intake, combined with mineral balance, produces outcomes neither of which is achieved independently. The synergy matters more than isolated nutrients.
This doesn’t require complicated protocols. Adequate protein consumption from varied sources, attention to magnesium status, and vitamin K2 from fermented foods or supplementation. Simple interventions with measurable skeletal benefits.

Cognitive Function: Macronutrients and Mental Performance
A high-fat meal increases your motivation to complete tasks. The same meal reduces your ability to switch between them.
This creates an impossible optimisation problem. You cannot maximise motivation and cognitive flexibility simultaneously through macronutrient manipulation. Prioritising one compromises the other. When you eat for different goals involving mental performance, accepting these trade-offs becomes necessary.
Water complicates this further. If you’re not thirsty, drinking impairs cognitive performance rather than improving it. Thirsty individuals show faster response times after drinking. Non-thirsty individuals slow down. The correction only works when dehydration exists.
Dietary patterns matter more than isolated nutrients for long-term cognitive health. The Mediterranean diet (olive oil, plant-based foods, fish-focused), DASH diet (blood-pressure–lowering eating plan), and MIND diet (brain-health eating plan) all demonstrate protective effects against cognitive decline. They share common elements: abundant plant foods, lean proteins, and healthy fats. No single nutrient explains the benefit. The pattern does.
Body weight extremes accelerate cognitive deterioration. Obesity in middle age increases dementia risk. Excessive weight loss in older adults speeds decline. Both overnutrition and undernutrition harm brain function through different mechanisms. The margin for error narrows with age.
Protein from diverse sources supports cognitive performance alongside physical health. Fish, soybean products, dairy. Not because of protein content alone, but because these foods deliver complementary nutrients the brain requires.
Glucose metabolism affects cognition differently depending on body composition. In lean individuals, stress elevates blood glucose and impairs mental performance. In those with obesity, high glucose occurs regardless of stress, masking acute effects.
No perfect macronutrient ratio exists for cognitive optimisation. Context determines strategy. Task type, hydration status, body composition, age, and metabolic health all modify outcomes. The goal dictates the fuel.

Overall Wellness: How to Eat for Different Goals to Build Your Foundation
Wellness isn’t a goal. It’s the baseline enabling every other goal.
Deficient in micronutrients? Fat loss stalls. Chronically dehydrated? Muscle growth plateaus. Ignoring fibre? Metabolic health deteriorates. Specific goals require foundations.
The Universal Requirements
Three elements support every nutritional strategy:
- Fibre: 30 grams daily from whole grains, vegetables, fruits, legumes
- Hydration: 1.5 ml per kilocalorie, approximately 2-3 litres daily
- Nutrient diversity: varied whole foods prevent isolated deficiencies better than supplementation
Simple lifestyle modifications combining proper nutrition with regular exercise prevent metabolic complications more effectively than isolated interventions. The combination outperforms either alone.
Individual Foundations Differ
Body composition, activity level, dietary restrictions, and sleep quality all modify baseline needs. Greek employees showed no correlation between BMI and water balance, demonstrating that individual hydration requirements transcend simple body mass metrics.
When you eat for different goals involving overall wellness, a personalised assessment identifies your specific foundation. The tool below generates targeted recommendations based on your health focus, activity patterns, dietary approach, and sleep quality.
- Calcium & Magnesium balance
- Vitamin D optimisation
- Omega-3 fatty acids
Meal Timing Flexibility
Training demands structured timing. General wellness permits adaptation. Aligning intake with circadian rhythms optimises metabolic health. Concentrating food within daylight hours supports natural hormone patterns.
Three balanced meals work. Six smaller occasions work. The pattern you sustain beats the theoretically optimal pattern you abandon.
Wellness nutrition prevents constraints undermining training response, stress recovery, or adaptive capacity. Build foundations first. Optimise goals second.
Your body responds to what you ask it to do. Fat loss, muscle gain, athletic performance, metabolic health, healthy ageing, bone preservation, cognitive function, overall wellness.
Each goal creates distinct physiological demands that nutrition must meet. The macronutrient ratios supporting fat loss undermine muscle gain. The timing strategies optimising endurance compromise strength adaptation.
The mineral balances that protect bone health differ from those that support metabolic function. When you eat for different goals, accepting these trade-offs and aligning nutrient intake with physiological priority determines whether effort produces adaptation or accumulates fatigue. No universal protocol exists. Your goal dictates your fuel.
Sources
- Alharazy S, Robertson MD, Lanham-New S, Naseer MI, Chaudhary AG, Alissa E. Directly measured free and total 25-hydroxyvitamin D levels in relation to metabolic health in multi-ethnic postmenopausal females in Saudi Arabia. Endocr Connect. 2021;10:1594–1606.
- American Dietetic Association; Dietitians of Canada; American College of Sports Medicine; Rodriguez NR, Di Marco NM, Langley S. American College of Sports Medicine position stand. Nutrition and athletic performance. Med Sci Sports Exerc. 2009 Mar;41(3):709-31.
- Antonio J, Candow DG, Forbes SC, et al. Common questions and misconceptions about creatine supplementation: what does the scientific evidence really show? J Int Soc Sports Nutr. 2021;18(1):13.
- Buondonno I, Sassi F, Carignano G, Dutto F, Ferreri C, Pili F, et al. From mitochondria to healthy ageing: the role of branched-chain amino acids treatment: a randomised study. Clin Nutr. 2020;39:2080–91.
- Celis‐Morales, C., Livingstone, K.M., Marsaux, C.F., Macready, A.L., Fallaize, R., O’Donovan, C.B. et al. (2017) Effect of personalised nutrition on health‐related behaviour change: evidence from the Food4Me European randomised controlled trial. International Journal of Epidemiology, 46(2), 578–588.
- Chandler RM, Byrne HK, Patterson JG, Ivy JL. Dietary supplements affect the anabolic hormones after weight-training exercise. J Appl Physiol. 1994;76:839–45.
- Chawla SPS, Kaur S, Bharti A, et al. Impact of health education on knowledge, attitude, practices and glycemic control in type 2 diabetes mellitus. J Family Med Prim Care. 2019;8(1):261–268.
- Cienfuegos S., Gabel K., Kalam F., Ezpeleta M., Wiseman E., Pavlou V., Lin S., Oliveira M.L., Varady K.A. Effects of 4- and 6-h Time-Restricted Feeding on Weight and Cardiometabolic Health: A Randomized Controlled Trial in Adults with Obesity. Cell Metab. 2020;32:366–378.e3.
- Dai Q, Shu XO, Deng X, Xiang YB, Li H, Yang G, Shrubsole MJ, Ji B, Cai H, Chow WH, et al. Modifying effect of calcium/magnesium intake ratio and mortality: A population-based cohort study. BMJ Open. 2013;3:e002111.
- de Vries J, Birkett A, Hulshof T, et al. Effects of cereal, fruit and vegetable fibers on human fecal weight and transit time: a comprehensive review of intervention trials. Nutrients. 2016;8(3):130.
- Dye L, Boyle NB, Champ C, Lawton C. The relationship between obesity and cognitive health and decline. Proc Nutr Soc. 2017;76:443–454.
- EFSA Scientific Opinion on Dietary Reference Values for water. EFSA J. 2010;8:1459.
- Ekingen T, Sob C, Hartmann C, Rühli FJ, Matthes KL, Staub K, Bender N. Associations between hydration status, body composition, sociodemographic and lifestyle factors in the general population: A cross-sectional study. BMC Public Health. 2022;22:900.
- Escobedo-Monge MF, Barrado E, Parodi-Roman J, Escobedo-Monge MA, Torres-Hinojal MC, Marugan-Miguelsanz JM. Magnesium status and Ca/Mg ratios in a series of children and adolescents with chronic diseases. Nutrients. 2022;14:2941.
- Forbes GB. Body composition in adolescence. Prog Clin Biol Res. 1981;61:55–72.
- Garthe I, Raastad T, Refsnes PE, et al. Effect of two different weight-loss rates on body composition and strength and power-related performance in elite athletes. Int J Sport Nutr Exerc Metab. 2011;21(2):97–104.
- Gutiérrez S, Svahn SL, Johansson ME. Effects of Omega-3 Fatty Acids on Immune Cells. Int J Mol Sci. 2019;20:5028.
- Hamilton, DL, Philp, A. Can AMPK mediated suppression of mTORC1 explain the concurrent training effect? Cell Mol Exerc Physiol. 2013;2(1):e4.
- Heileson JL, Elliott A, Buzzard JA, et al. A Cross-sectional analysis of whole blood long-chain ω-3 polyunsaturated fatty acids and its relationship with dietary intake, body composition, and measures of strength and power in collegiate athletes. J Am Nutr Assoc. 2023;42(1):94–100.
- Houston D, Nicklas B, Ding J, Harris T, Tylavsky F, Newman A, et al. Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the health, aging, and body composition (health ABC) study. Am J Clin Nutr. 2008;87:150–5.
- Imamura F, Micha R, Wu JHY, de Oliveira Otto MC, Otite FO, Abioye AI, Mozaffarian D. Effects of Saturated Fat, Polyunsaturated Fat, Monounsaturated Fat, and Carbohydrate on Glucose-Insulin Homeostasis: A Systematic Review and Meta-analysis of Randomised Controlled Feeding Trials. PLoS Med. 2016;13:e1002087.
- Kerksick CM, Wilborn CD, Roberts MD, et al. ISSN exercise & sports nutrition review update: research & recommendations. J Int Soc Sports Nutr. 2018;15:38.
- Kerstetter JE, Caseria DM, Mitnick ME, Ellison AF, Gay LF, Liskov TA, Carpenter TO, Insogna KL. Increased Circulating Concentrations of Parathyroid Hormone in Healthy, Young Women Consuming a Protein-Restricted Diet. Am J Clin Nutr. 1997;66:1188–1196.
- Kerstetter JE, O’Brien KO, Caseria DM, Wall DE, Insogna KL. The Impact of Dietary Protein on Calcium Absorption and Kinetic Measures of Bone Turnover in Women. J Clin Endocrinol Metab. 2005;90:26–31.
- Koutsos, A., Griffin, B.A., Antoni, R., Ozen, E., Sellem, L., Wong, G. et al. (2024) Variation of LDL cholesterol in response to the replacement of saturated with unsaturated fatty acids: a nonrandomised, sequential dietary intervention; the Reading, Imperial, Surrey, saturated fat cholesterol intervention (“RISSCI”‐1) study. The American Journal of Clinical Nutrition, 120(4), 854–863.
- Kreider R.B. Effects of creatine supplementation on performance and training adaptations. Mol. Cell Biochem. 2003;244:89–94.
- Kreider RB, Kalman DS, Antonio J, et al. International society of sports nutrition position stand: Safety and efficacy of creatine supplementation in exercise, sport, and medicine. J Int Soc Sports Nutr. 2017;14(1):18.
- Kriengsinyos W, Wykes LJ, Goonewardene LA, Ball RO, Pencharz PB. Phase of menstrual cycle affects lysine requirement in healthy women. Am J Physiol Endocrinol Metab. 2004;287:E489–E496.
- Kyrou I, Tsigos C. Stress hormones: physiological stress and regulation of metabolism. Current Opinion in Pharmacology. 2009;9(6):787–793.
- Harris, S. Hamilton, L.B. Azevedo, J. Olajide, C. De Brún, G. Waller, et al. Intermittent fasting interventions for treatment of overweight and obesity in adults: a systematic review and meta-analysis. JBI Database System Rev Implement Rep, 16 (2) (2018), pp. 507-547.
- Lemon PWR. Beyond the zone: Protein needs of active individuals. J Am Coll Nutr. 2000;19:513S–21S.
- Longland TM, Oikawa SY, Mitchell CJ, et al. Higher compared with lower dietary protein during an energy deficit combined with intense exercise promotes greater lean mass gain and fat mass loss: A randomised trial. Am J Clin Nutr. 2016;103(3):738–746.
- Morton R.W., Murphy K.T., McKellar S.R., Schoenfeld B.J., Henselmans M., Helms E., Aragon A.A., Devries M.C., Banfield L., Krieger J.W., et al. A Systematic Review, Meta-Analysis and Meta-Regression of the Effect of Protein Supplementation on Resistance Training-Induced Gains in Muscle Mass and Strength in Healthy Adults. Br. J. Sports Med. 2018;52:376–384.
- Munger RG, Cerhan JR, Chiu BC. Prospective Study of Dietary Protein Intake and Risk of Hip Fracture in Postmenopausal Women. Am J Clin Nutr. 1999;69:147–152.
- Pennings B, Groen B, de Lange A, et al. Amino acid absorption and subsequent muscle protein accretion following graded intakes of whey protein in elderly men. Am J Physiol Endocrinol Metab, 302 (2012), p. 992
- Rogers PJ, Kainth A, Smit HJ. A drink of water can improve or impair mental performance depending on small differences in thirst. Appetite. 2001;36:57-58.
- Scarmeas N, Anastasiou CA, Yannakoulia M. Nutrition and prevention of cognitive impairment. Lancet Neurol. 2018;17:1006–1015.
- Seino S, Sumi K, Narita M, Yokoyama Y, Ashida K, Kitamura A, Shinkai S. Effects of Low-Dose Dairy Protein Plus Micronutrient Supplementation during Resistance Exercise on Muscle Mass and Physical Performance in Older Adults: A Randomised, Controlled Trial. J Nutr Health Aging. 2018;22(1):59-67.
- Slimani M, Nikolaidis PT. Anthropometric and physiological characteristics of male Soccer players according to their competitive level, playing position and age group: a systematic review. J Sports Med Phys Fitness. 2017;59(1):141–163.
- Thomas DT, Erdman KA, Burke LM. American College of Sports Medicine Joint Position Statement. Nutrition and Athletic Performance. Med Sci Sports Exerc. 2016;48:543–568.
- Uwitonze AM, Razzaque MS. Role of magnesium in vitamin D activation and function. J Am Osteopath Assoc. 2018;118:181–189.
- van den Hoek A, Zondag G, Verschuren L, de Ruiter C, Attema J, de Wit E, et al. A novel nutritional supplement prevents muscle loss and accelerates muscle mass recovery in caloric-restricted mice. Metabolism. 2019;97:57–67.
- Volpe SL. Magnesium in Disease Prevention and Overall Health. Adv Nutr Int Rev J. 2013;4:378S–383S.
- Von Haehling S, Morley JE, Anker SD. An overview of sarcopenia: Facts and numbers on prevalence and clinical impact. J Cachexia Sarcopenia Muscle. 2010;1:129–133.
- Wagenaar CA, Dekker LH, Navis GJ. Prevalence of sarcopenic obesity and sarcopenic overweight in the general population: The lifelines cohort study. Clin Nutr. 2021;40:4422–4429.
- World Health Organization, Diabetes, fact sheet.
- Yang J., Park H.J., Hwang W., Kim T.H., Kim H., Oh J., Cho M.S. Changes in the glucose and insulin responses according to high-protein snacks for diabetic patients. Nutr. Res. Pract. 2021;15:54–65.
- Zembron-Lacny A, Morawin B, Wawrzyniak-Gramacka E, Gramacki J, Jarmuzek P, Kotlega D, Ziemann E. Multiple Cryotherapy Attenuates Oxi-Inflammatory Response Following Skeletal Muscle Injury. Int J Environ Res Public Health. 2020 Oct 27;17(21):7855.



