Minerals micronutrient balance forms an essential foundation for human health, affecting nearly every physiological process in the body. These inorganic (non-carbon-containing) elements, required in varying amounts, regulate enzyme functions, maintain fluid balance, support nerve signalling, and contribute to bone formation.
Unlike vitamins, minerals remain stable during cooking and food processing. However, various dietary factors can affect their bioavailability (proportion absorbed and utilised by the body).
Approximately thirty essential minerals micronutrient elements support normal physiological function, with requirements changing throughout different life stages. These elements influence biological processes, including metabolism (chemical reactions in the body), enzyme function, hormonal regulation, and other vital activities.
The classification of minerals into macro (needed in more significant amounts, >100mg daily) and micro (needed in smaller quantities, <100mg daily) categories helps distinguish their roles and required amounts.
Despite their importance, suboptimal mineral intake below recommended dietary allowances remains common, even in industrialised countries. This nutritional gap can directly impact energy levels, cognitive performance, and general well-being. The interrelationship between numerous minerals in metabolic pathways suggests that proper mineral balance, rather than single-nutrient focus, offers the most significant health benefits.
The scientific understanding of mineral nutrition has evolved significantly over recent decades, with updated guidelines reflecting new discoveries about mineral functions, interactions, and optimal intake levels. This growing knowledge has transformed approaches to addressing deficiencies and maintaining mineral balance for optimal health.
In the following sections, we’ll explore the classification and roles of these essential nutrients, examine the health impacts of deficiencies and toxicities, present a comprehensive reference table, discuss factors affecting bioavailability, and trace how our understanding of mineral nutrition has evolved.
Understanding Minerals Micronutrient Classification and Roles
The human body requires minerals in varying amounts to maintain optimal function. These inorganic elements cannot be synthesised (produced naturally) within the body and must be obtained through dietary sources. Minerals micronutrient elements are categorised based on daily requirements, reflecting their distinct roles in physiological processes.
Minerals originate primarily in water, topsoil, plant root systems, and animal tissues that consume mineral-containing plants and water. Their presence throughout natural ecosystems highlights their fundamental importance to all life forms. The human body has evolved to utilise these elements precisely for structure, function, and regulation.
Classification of Essential Minerals
The classification of minerals helps scientists and healthcare professionals categorise these elements according to the body’s requirements and physiological roles. Understanding these classifications provides insight into how different minerals uniquely contribute to bodily functions.
1: Macrominerals (Required >100mg daily)
The body needs these minerals in greater amounts, and they play primary roles in structural support, fluid balance, and significant metabolic processes.
- Calcium: Forms bone structure, enables muscle contraction, supports nerve signalling
- Phosphorus: Essential for bone mineralisation, energy production (ATP), and DNA structure
- Magnesium: Serves as an enzyme cofactor that supports muscle and nerve function
- Sodium: Maintains fluid balance, enables nerve impulse transmission
- Potassium: Regulates heart rhythm, supports muscle function, balances fluids
- Chloride: Forms stomach acid, maintains acid-base balance
- Sulphur: Contributes to protein structure and supports detoxification processes
2: Microminerals/Trace Minerals (Required <100mg daily)
These minerals are needed in smaller amounts but are equally essential for health, often as critical components in enzymes and specialised proteins.
- Iron: Transports oxygen via haemoglobin (oxygen-carrying protein in blood), supports energy metabolism
- Zinc: Enables immune function, wound healing, DNA synthesis
- Copper: Assists iron metabolism, supports connective tissue formation
- Iodine: Required for thyroid hormone synthesis
- Selenium: Functions as an antioxidant, supports thyroid metabolism
- Manganese: Acts as an enzyme cofactor that supports bone formation
- Fluoride: Strengthens tooth enamel, supports bone health
- Chromium: May enhance insulin function (status debated)
- Molybdenum: Serves as an enzyme cofactor in detoxification
Structural Functions
Minerals micronutrient elements provide crucial structural support throughout the body. Calcium and phosphorus form the crystalline structure (mineral arrangement) of bones and teeth, with approximately 99% of body calcium stored in these hard tissues. Magnesium also contributes to bone structure, while sulphur forms disulphide bridges (chemical bonds between protein portions) that maintain protein shape, particularly in hair, skin, and nails.
The skeletal system requires a balance of multiple minerals to maintain proper density and strength. Research demonstrates that imbalances in the calcium-to-phosphorus ratio can impact bone mineralisation (the process of incorporating minerals into the bone matrix) and overall skeletal health. These structural roles explain why adequate mineral intake remains important during growth periods and prevents age-related bone loss.
Regulatory Functions
In addition to structural roles, minerals regulate countless physiological processes through various mechanisms:
Enzymatic Regulation
- Serve as cofactors for over 600 enzymes
- Enable reactions for energy production and metabolism
- Support DNA/RNA (deoxyribonucleic acid/ribonucleic acid, genetic material) synthesis and repair
- Facilitate protein formation
Fluid and Electrolyte Balance
- Maintain appropriate cellular hydration
- Regulate blood pressure and volume
- Support acid-base balance
- Enable nerve signal transmission
Hormone Production and Function
- Essential for thyroid hormone synthesis (iodine)
- Support insulin action (chromium)
- Influence reproductive hormone production
- Affects stress hormone regulation
Metabolic Functions
Minerals play vital roles in energy metabolism and oxygen transport. Iron forms the central component of haemoglobin (oxygen-carrying protein in red blood cells), enabling oxygen delivery to tissues. B vitamins and minerals like iron, magnesium, and zinc participate directly in energy-yielding pathways, affecting physical performance and daily energy levels.
The electron transport chain (series of protein complexes that generate cellular energy), which produces cellular energy, requires several minerals as essential components. Copper, iron, and manganese serve as electron carriers. At the same time, magnesium activates ATP (adenosine triphosphate, the central energy molecule in cells), the primary energy currency of cells. These processes highlight why mineral deficiencies often manifest as fatigue and reduced exercise capacity.
Protective Functions
Several minerals provide protective benefits through antioxidant mechanisms. Selenium, copper, zinc, and manganese function within antioxidant enzyme systems that neutralise damaging free radicals. These protective functions help prevent cellular damage and may reduce chronic disease risk.
The immune system relies heavily on mineral availability, with zinc particularly important for immune cell development and function. Research demonstrates that zinc supplementation can shorten illness duration and improve survival in specific populations. This protective role explains why maintaining adequate mineral status supports overall resilience against environmental challenges.
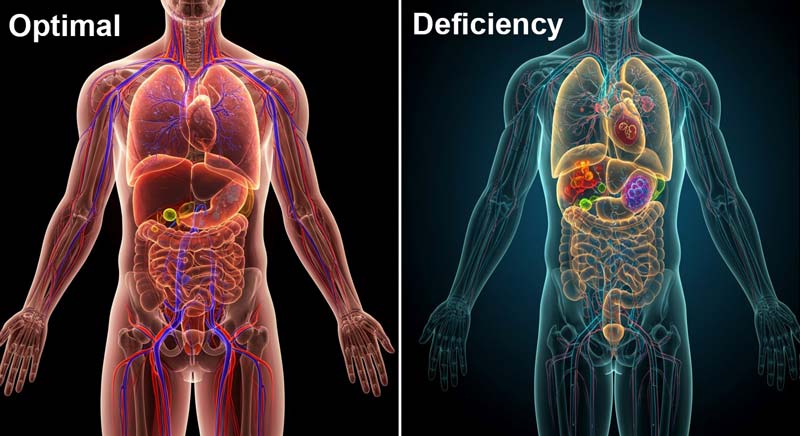
Health Impacts of Mineral Deficiency and Toxicity
Mineral balance represents a delicate equilibrium within the human body. Deficiencies and excesses can trigger widespread health consequences affecting nearly every body system.
This balance becomes particularly important as minerals micronutrient elements interact, creating synergistic or antagonistic relationships that affect absorption and utilisation.
The health implications of imbalances often develop gradually, with subtle symptoms appearing before more serious manifestations. These gradual changes can make identification challenging without appropriate testing and assessment. Minerals micronutrient status assessment helps identify potential imbalances early and guides appropriate interventions.
Bone and Skeletal Health
Mineral deficiencies significantly impact skeletal structure and function:
Calcium Deficiency
- Reduced bone density and increased fracture risk
- Impaired muscle contraction and cramping
- Altered nerve function affecting coordination
Phosphorus Imbalance
- Too little: Weakened bone structure and poor mineralisation
- Too much: Disrupted calcium balance and soft tissue calcification
Magnesium Insufficiency
- Altered bone crystal formation
- Reduced calcium absorption and metabolism
- Increased risk of osteoporosis in combination with other deficiencies
Studies demonstrate that the relationship between minerals and skeletal health involves multiple nutrients. The calcium-to-magnesium ratio plays a crucial role in bone health, with imbalances affecting bone remodelling and mineralisation. Long-term imbalances are associated with increased osteoporosis risk and fracture incidence.
Cardiovascular System Effects
Mineral status directly influences heart function and vascular health:
Potassium and Sodium Balance
- Regulates blood pressure through fluid balance
- Affects heart rhythm and contraction force
- Imbalances increase hypertension and stroke risk
Magnesium Status
- Supports normal cardiac conduction
- Helps regulate vascular tone
- Deficiency linked to arrhythmias and hypertension
Iron Considerations
- Necessary for oxygen transport via haemoglobin
- Both deficiency and excess can impact heart function
- Low levels cause compensatory increased heart rate
Research indicates that potassium and magnesium inadequacy may increase the risk of hypertension and cardiovascular diseases. Public health efforts increasingly focus on sodium reduction and potassium enhancement to improve population cardiovascular health outcomes.
Immune Function and Resilience
Several minerals directly support immune system operation:
Zinc Importance
- Essential for immune cell development and function
- Supports wound healing and tissue repair
- Deficiency increases infection susceptibility
Selenium Roles
- Forms part of antioxidant enzymes protecting immune cells
- Supports thyroid function, which affects immunity
- It may reduce viral infection severity
Iron Balance
- Required for immune cell proliferation
- Both deficiency and excess affect infection risk
- Carefully managed in areas with endemic infections
Studies show that zinc plays a crucial role in immune function, with supplementation offering benefits in various clinical scenarios, including reducing the duration of common illnesses and supporting recovery from infections. This evidence highlights the practical application of mineral nutrition knowledge in health maintenance.
Neurological and Cognitive Effects
Brain function relies heavily on proper mineral status:
Iodine Requirements
- Essential for thyroid hormones that drive brain development
- Deficiency causes intellectual impairment if present during development
- Adult deficiency impairs cognitive function and energy levels
Iron Needs
- Supports neurotransmitter production
- Enables proper myelination of nerve cells
- Deficiency linked to attention and learning difficulties
Magnesium Functions
- Regulates neurotransmitter release
- Supports brain energy metabolism
- Deficiency associated with neurological excitability
Minerals influence cognitive development and function in various ways. Research demonstrates that inadequate mineral nutrition during critical developmental periods can affect cognitive capabilities. Even in adults, correcting deficiencies can improve cognitive performance and mood regulation.
Metabolic and Endocrine Impacts
Hormone production and metabolism depend on mineral availability:
Chromium Considerations
- It may enhance insulin sensitivity and glucose regulation
- Deficiency potentially impairs glucose tolerance
- Research continues regarding the essential status
Iodine Requirements
- Forms critical component of thyroid hormones
- Deficiency causes goitre and hypothyroidism (underactive thyroid condition)
- Excess can paradoxically (unexpectedly) suppress thyroid function
Selenium Needs
- Activates thyroid hormones through deiodinase enzymes
- Works synergistically with iodine for thyroid function
- Balance is essential for optimal metabolism
Magnesium inadequacy has been associated with type-2 diabetes and affects insulin sensitivity. Research indicates that maintaining proper magnesium status may help prevent metabolic disorders and support glucose regulation, highlighting the importance of this mineral in metabolic health.
Toxicity Concerns
While deficiencies cause numerous health problems, excessive mineral intake can also create significant issues:
Selenium Toxicity
- The upper limit was recently lowered based on evidence linking high intake to hair loss.
- Long-term high intake may impair immune function
- Supplements require careful dosing
Iron Overload
- It can damage the liver, heart, and endocrine organs
- This is particularly problematic in genetic conditions like haemochromatosis (iron storage disorder)
- Supplementation requires appropriate testing and monitoring
Zinc Excess
- High doses cause copper deficiency
- May impair immune function paradoxically
- Can lower beneficial HDL cholesterol levels
Reviews have reassessed safe upper limits for several minerals. For example, the European Food Safety Authority proposed lowering the adult selenium upper limit to 255 µg/day after noting studies linking intakes above 300 µg with alopecia. These evolving guidelines reflect a growing understanding of mineral toxicity mechanisms.
Comprehensive Minerals Micronutrient Reference Table
Organised information about the full spectrum of minerals micronutrient requirements, functions, and implications provides valuable guidance. This comprehensive reference presents essential data about mineral nutrition in an accessible format.
The table below is a practical guide for assessing mineral status, identifying potential imbalances, and making informed dietary choices.
The reference data synthesises findings from numerous scientific studies and nutritional authorities. This information represents consensus guidelines rather than isolated research, providing reliable benchmarks for mineral nutrition. Updates to these guidelines occur periodically as scientific knowledge advances.
Minerals Micronutrient Reference Guide
µg = micrograms | mg = milligrams | UL = Tolerable Upper Intake Level (maximum daily safe intake)
Detailed analysis of 15 essential minerals across 7 key metrics, including daily requirements, primary functions, and deficiency symptoms. This comprehensive minerals micronutrient reference highlights absorption factors and meaningful nutrient interactions for maintaining physiological balance.
The Table Components Explained
Daily Requirement
This represents the recommended intake for healthy adults, though specific needs vary based on age, sex, and life stage. When RDA cannot be determined, these values typically reflect the Recommended Dietary Allowance (RDA) or Adequate Intake (AI). Requirements often increase during pregnancy, lactation, and for athletes with higher metabolic demands.
Primary Functions
Each mineral serves specific physiological roles, though many participate in multiple systems simultaneously. These functions range from structural support (bones, teeth) to enzyme activation and hormone production. These roles help explain the varied symptoms that can develop when imbalances occur.
Deficiency Symptoms
Inadequate mineral intake or absorption leads to predictable patterns of dysfunction. Early symptoms often appear subtle and nonspecific, while advanced deficiencies cause more recognisable clinical signs. These manifestations reflect the disruption of the mineral’s primary functions in the body.
Toxicity & Upper Limits
Excessive mineral intake can cause adverse effects ranging from mild digestive upset to severe organ damage. Upper Limits (UL) represent the highest intake and are unlikely to cause harm in most individuals. These limits apply to total intake from food and supplements combined, with supplemental forms typically presenting higher risk due to concentrated delivery.
Best Food Sources
Dietary sources vary in mineral content and bioavailability. Plant foods contain minerals reflecting the soil composition where they grew. In contrast, animal products contain minerals accumulated through the food chain. The richest sources often include:
- Leafy greens: Calcium, magnesium, iron
- Nuts and seeds: Zinc, selenium, magnesium
- Whole grains: Phosphorus, magnesium, selenium
- Seafood: Iodine, selenium, zinc
- Meats and poultry: Iron, zinc, phosphorus
- Dairy products: Calcium, phosphorus, potassium
Bioavailability Factors
Mineral absorption varies significantly based on several factors. Bioavailability refers to the proportion of a nutrient absorbed and utilised by the body. For minerals, this can be affected by:
- Chemical form: Some forms absorb more readily than others
- Dietary components: Certain substances enhance or inhibit absorption
- Nutritional status: Deficiency sometimes increases absorption efficiency
- Age and health condition: Absorption capacity changes throughout life
- Medication use: Some drugs affect mineral utilisation
For example, vitamin C enhances non-heme iron absorption. At the same time, phytates in whole grains can bind minerals and reduce their availability. These factors help explain why meeting recommended intake levels sometimes fails to achieve optimal mineral status.
Nutrient Interactions
Minerals interact with each other and with vitamins in ways that affect overall nutritional status:
Synergistic Relationships
- Vitamin D enhances calcium absorption
- Vitamin C improves iron uptake
- Selenium works with iodine for thyroid function (hormone production by the thyroid gland)
Competitive Interactions
- Zinc competes with copper for absorption
- High calcium intake can reduce iron and zinc availability
- Excess manganese affects iron metabolism
Balance Requirements
- The calcium-to-phosphorus ratio affects bone health.
- Sodium-to-potassium balance influences blood pressure
- The zinc-to-copper proportion impacts immune function
Research demonstrates that these interactions have practical implications. For instance, the calcium-to-magnesium ratio should ideally remain around 2:1 for optimal physiological effects. Imbalanced ratios may affect bone health, cardiovascular function, and metabolic processes.
Applications Across Life Stages
Childhood and Adolescence
Mineral requirements increase during growth periods to support development. Calcium, phosphorus, and magnesium must peak during adolescent growth spurts to support rapid bone formation. Zinc becomes particularly important for growth and sexual maturation during puberty. At the same time, iron needs increase with muscle development and blood volume expansion.
Pregnancy and Lactation
Mineral requirements adjust significantly during reproduction. Iron must nearly double during pregnancy to support increased blood volume and foetal development. Calcium and magnesium requirements increase to support foetal skeletal development while maintaining maternal bone health. Iodine becomes particularly crucial for foetal brain development, with deficiencies causing permanent intellectual impairment.
Ageing Population
Older adults face unique mineral nutrition challenges. Absorption efficiency often decreases with age, while medication use may further affect mineral status. Calcium and vitamin D need to increase to combat age-related bone loss, particularly in postmenopausal women. As natural immunity declines with age, zinc and selenium status become essential for maintaining immune function.
Athletic Performance
Physical activity affects mineral requirements in specific ways. Increased sweat losses necessitate higher intakes of electrolytes like sodium, potassium, and magnesium. Iron demands rise to support expanded blood volume and enhanced oxygen transport capacity. Zinc must increase to support tissue repair and immune function during intense training.
Practical Assessment Considerations
Blood work provides valuable insight into minerals micronutrient status, though interpretation requires knowledge of normal variations. Standard blood tests may assess:
- Serum calcium and phosphorus
- Ferritin and haemoglobin (iron status)
- Serum zinc and copper
- Thyroid function (indirect iodine assessment)
However, blood levels don’t always reflect total body stores or functional status. For example, serum magnesium remains normal even when intracellular levels decline, making deficiency challenging to detect through standard testing. Comprehensive assessment may require specialised testing for specific minerals.
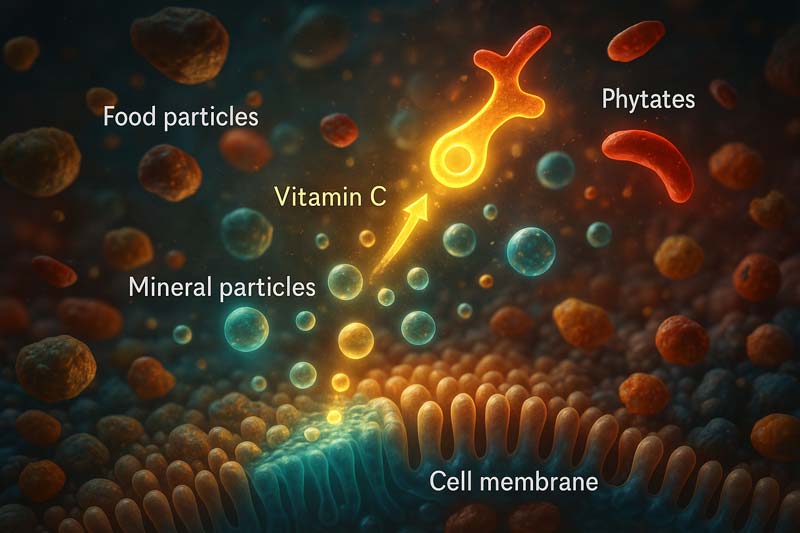
Bioavailability Factors and Nutrient Interactions
The presence of minerals micronutrient elements in food does not guarantee their absorption and utilisation by the body. Bioavailability, the proportion of an ingested nutrient that becomes available for physiological functions, varies widely based on numerous factors. These variations help explain why meeting recommended intake levels sometimes fails to achieve optimal mineral status.
Mineral absorption occurs primarily in the small intestine through specialised mechanisms. Some minerals micronutrient elements share absorption pathways, creating competition for uptake. In contrast, others require specific carriers or environmental conditions for optimal absorption. These physiological realities create a dynamic picture of mineral nutrition beyond simple intake values.
Dietary Enhancers and Inhibitors
Several dietary components can either enhance or inhibit mineral absorption. These factors significantly influence how much mineral the body uses after consumption.
Absorption Enhancers
- Vitamin C: Increases non-haem iron absorption by converting it to more soluble forms
- Organic acids: Citric, malic, and lactic acids improve mineral solubility
- Animal protein: Contains amino acids that form soluble complexes with minerals
- Vitamin D: Enhances calcium and phosphorus absorption in the intestine
- Healthy gut bacteria: Produces short-chain fatty acids that improve mineral uptake
Absorption Inhibitors
- Phytates: Found in whole grains, legumes, and nuts; bind minerals like zinc, iron, and calcium
- Oxalates: Present in spinach, rhubarb, and tea; reduce calcium absorption
- Polyphenols: In tea, coffee, and wine, decrease iron availability
- Excessive fibre: Can trap minerals and reduce absorption efficiency
- Calcium supplements: When taken in large doses, may inhibit iron and zinc uptake
Research demonstrates that strategic food combinations can significantly affect mineral absorption. For example, adding vitamin C-rich foods to plant-based iron sources can increase iron absorption by 3-6 times. Similarly, soaking, sprouting, or fermenting grains and legumes reduces their phytate content, enhancing mineral bioavailability.
Mineral-Mineral Interactions
Minerals interact with each other in ways that affect overall nutritional status:
Competitive Interactions
- Zinc and Copper: High zinc intake reduces copper absorption
- Iron and Manganese: Compete for binding sites during absorption
- Calcium and Magnesium: Large calcium doses can reduce magnesium uptake
- Phosphorus and Calcium: Excessive phosphorus can affect calcium metabolism
Synergistic Relationships
- Selenium and Iodine: Work together for optimal thyroid function
- Potassium and Magnesium: Support each other’s roles in heart function
- Copper and Iron: Copper helps mobilise iron for haemoglobin synthesis
These interactions create practical considerations for supplementation and dietary planning. For example, the established 40 mg Upper Limit for zinc was set to prevent copper deficiency. These relationships help explain why isolated high-dose supplementation of single minerals can sometimes create unexpected imbalances.
The Critical Balance Ratios
Certain mineral pairs function optimally when consumed in specific proportions:
Calcium Ratio
- Ideal ratio: Approximately 2:1
- Implications: Affects bone health, muscle function, and cardiovascular health
- Balancing strategy: Include abundant magnesium-rich foods when calcium intake is high
Studies reveal that an imbalanced calcium ratio can exacerbate metabolic disorders. Research demonstrates that persons with poorly controlled type 2 diabetes often have higher calcium ratios than those with better control. This finding suggests that mineral balance affects health outcomes, not just absolute intake.
Sodium Ratio
- Modern diet issue: Typically too high in sodium, too low in potassium
- Health effects: Influences blood pressure and fluid balance
- Recommendation: Increase potassium-rich whole foods while reducing processed food intake
Research supports focusing on the sodium ratio rather than sodium alone for cardiovascular health. Public health strategies increasingly emphasise potassium-enriched salt substitutes to improve this ratio in population-level interventions.
Zinc Ratio
- Balance concern: High-dose zinc supplements can induce copper deficiency
- Monitoring needs: Long-term zinc supplementation requires copper status assessment
- Practical guideline: Copper supplementation may be necessary with extended zinc therapy
Physiological and Individual Factors
Bioavailability varies significantly between individuals based on several factors:
Life Stage Influences
- Pregnancy: Increased absorption efficiency for iron and calcium
- Growth periods: Enhanced uptake of minerals for development
- Ageing: Reduced absorption capacity, particularly for calcium and vitamin B12
Health Status Effects
- Iron deficiency: Stimulates increased absorption capacity
- Gastrointestinal disorders May impair the uptake of multiple minerals
- Specific genetic variations Affect transport protein function and efficiency
Medication Interactions
- Proton pump inhibitors: Reduce acid-dependent mineral absorption
- Certain antibiotics: Form complexes with minerals, preventing absorption
- Diuretics: Affect mineral retention and excretion patterns
Research indicates that identical twins can have different mineral absorption capacities based on gut microbiome differences and environmental exposures. This individualised aspect of mineral nutrition supports the value of personalised assessment and tailored recommendations.
Optimisation Strategies
Several evidence-based approaches can enhance mineral bioavailability:
Food Preparation Methods
- Soaking: Reduces phytate content in beans, grains, and seeds
- Fermentation: Activates enzymes that break down absorption inhibitors
- Sprouting: Decreases phytates while increasing vitamin content
- Cooking techniques: Affect mineral retention and availability differently
Timing Considerations
- Supplement separation: Take calcium supplements at different times than iron
- Meal pairing: Consume vitamin C-rich foods with plant-based iron sources
- Spacing doses: Divide larger mineral supplements throughout the day
Source Selection
- Mineral forms: Some are better absorbed (e.g., ferrous iron over ferric forms)
- Food diversity: Provides minerals in various binding environments
- Fortified products: Often contain highly bioavailable mineral forms
Studies show that these practical approaches can significantly increase mineral absorption. For example, consuming meat, fish, or poultry with plant-based iron sources can improve non-haem iron absorption by 2-3 times through what’s known as the “meat factor” effect.

Historical Evolution of Mineral Nutrition Guidelines
Knowledge of minerals and micronutrient nutrition has radically transformed over the past several decades. Guidelines and recommendations have evolved as scientific knowledge has expanded, research methodologies have improved, and population health patterns have shifted.
This historical perspective provides context for current recommendations and hints at future directions in minerals micronutrient science.
Early mineral nutrition focuses primarily on preventing overt deficiency diseases like goitre (iodine deficiency) and anaemia (iron deficiency). However, as these essential deficiencies became less common in developed nations, attention shifted toward optimising health and preventing chronic disease through appropriate mineral intake.
Shifting Guideline Parameters
Official mineral intake recommendations have been periodically revised as evidence has evolved. These changes reflect growing scientific knowledge and changing population needs:
Calcium Guidelines
- Earlier focus: Basic bone health maintenance
- Current emphasis: Osteoporosis prevention, life-stage requirements
- Notable shift: Recognition that excessive supplementation confers limited benefit
Iron Recommendations
- Past approach: General population guidelines
- Current strategy: Sex and age-specific targets accounting for menstrual losses
- Key refinement: RDA for women increased from 15 to 18 mg to better cover menstrual losses
Zinc Parameters
- Prior recommendation: Higher intake levels for all groups
- Updated guidance: Reduced from 15 mg to 11 mg for men based on balance studies
- Safety emphasis: Established 40 mg Upper Limit to prevent copper deficiency
Sodium Guidelines
- Historical approach: 2.4 g target
- Current direction: Progressive reduction targets (<2.3 g/day)
- Framework change: Replaced Upper Limit with Chronic Disease Risk Reduction intake
Magnesium Standards
- Earlier recommendations: 350 mg for adult males
- Updated guidance: Increased to 420 mg based on metabolic needs
- Recognition factor: Widespread inadequacy identified in population surveys
These evolutionary changes demonstrate how mineral nutrition science continuously refines its recommendations based on expanding evidence. The modifications aren’t merely numerical adjustments but reflect more profound knowledge of how these nutrients function in the body and affect long-term health outcomes.
Newly Discovered Functions
Scientific advances have uncovered additional roles for certain minerals, expanding our appreciation of their importance:
Selenium Functions
- Traditional view: Primarily, antioxidant functions
- Expanded knowledge: Critical role in thyroid hormone activation
- Clinical relevance: Greater appreciation of selenium in thyroid health and interactions with iodine status
Zinc Roles
- Earlier focus: Growth and enzyme functions
- Additional recognition: Critical influence on immune response
- Application outcome: WHO/UNICEF recommendation for zinc in diarrhoea management (2004)
Copper Significance
- Classical perspective: Basic enzyme cofactor roles
- Emerging importance: Neurodevelopmental functions
- Current investigation: Possible links between marginal copper status and cognitive decline
Magnesium Involvement
- Traditional view: Primarily structural and enzymatic roles
- Expanding recognition: Involvement in metabolic syndrome and diabetes
- Clinical implications: Research into magnesium supplementation for glucose control
These discoveries highlight how mineral nutrition remains an active research area, with clinical applications continuously emerging from basic science investigations. Each new function identified enhances our appreciation of the importance of these essential nutrients.
Changing Toxicity Perspectives
As knowledge of mineral toxicity has grown, safety guidelines have been re-evaluated:
Selenium Safety
- Past Upper Limit: 400 µg (set in 2000)
- New evidence: Studies linking intakes >300 µg with hair loss
- Guideline adjustment: The European Food Safety Authority (EFSA, European Union’s food safety regulatory body) proposed lowering adult UL to 255 µg/day
Calcium Considerations
- Traditional focus: Maximising intake for bone health
- Emerging concern: Possible slight increase in cardiovascular risk with high-dose supplements
- Practice shift: Emphasis on food sources over supplements except for those with low intake
Manganese Monitoring
- Standard Upper Limit: 11 mg
- Refined guidance: Some countries advise lower intakes for older adults
- Safety rationale: Ageing decreases manganese excretion, increasing the risk of neurotoxic accumulation
Chromium Status
- Historical view: Essential trace element for insulin action
- Current questioning: The 2014 EFSA review found no definitive evidence of essentiality
- Ongoing debate: Research continues on chromium’s status as an essential nutrient
These evolving perspectives on toxicity demonstrate the importance of continuing safety assessment. As supplement use becomes more widespread, knowledge of both the benefits and risks of higher-dose mineral intake becomes increasingly essential for public health.
Public Health Initiatives
The past few decades have seen significant public health programmes to address mineral deficiencies globally:
Iodine Fortification
- Initiative timing: Spurred by the 1990 World Summit for Children
- Implementation approach: Universal salt iodisation
- Outcome success: Reduction in iodine-deficient countries from 110+ in 1993 to <20 today
Iron Fortification
- Programme expansion: Cereals and flour fortification became standard in many countries.
- Target population: Particularly aimed at reducing anaemia in women and children
- Mixed results: While progress occurred, iron deficiency anaemia remains common globally
Zinc Interventions
- Evidence-based timing: The following research in the late 1990s on zinc’s role in child growth
- Targeted approaches: Supplementation in children and fortification in staples
- Focus regions: Countries with high risk of zinc deficiency (South Asia, sub-Saharan Africa)
Fluoride Addition
- Historical context: Recognised since the mid-20th century for cavity prevention
- Implementation growth: Expanded to ~70% of the world’s table salt or water by 2000
- Current status: Continues but with careful monitoring to prevent fluorosis
These public health initiatives mark a shift from treating acute deficiencies to preventive nutrition strategies. Their success demonstrates how evidence-based mineral nutrition interventions can produce widespread population health benefits when implemented effectively.
Scientific Debates and Future Directions
Several key debates continue to shape the field of mineral nutrition:
Optimal Intake Levels
- Central question: What levels prevent deficiency versus optimise health?
- Evolving framework: Moving past deficiency prevention toward chronic disease reduction
- Research challenge: Determining the ideal intake for longevity and healthspan
Personalised Recommendations
- Current limitation: Population-based guidelines may not suit all individuals
- Emerging approach: Tailoring recommendations based on genetics, life stage, and health status
- Future direction: Precision nutrition accounting for individual absorption differences
Ultra-Trace Elements
- Research interest: Boron, silicon, and other non-essential elements
- Potential benefits: Possible roles in bone health or collagen formation
- Evidence status: Insufficient data for formal recommendations currently
Mineral Interactions with Microbiome
- New frontier: How gut bacteria affect mineral availability and vice versa
- Practical implications: Potential probiotic approaches to enhance mineral nutrition
- Research need: Better understanding of these bidirectional relationships
These ongoing scientific conversations will likely shape future mineral nutrition recommendations. As research methodologies advance and longer-term studies complete, our knowledge of optimal mineral intake will evolve increasingly nuancedly.
Sources
- Akimbekov N.S., Coban S.O., Atfi A., Razzaque M.S. The role of magnesium in pancreatic beta-cell function and homeostasis. Front. Nutr. 2024;11:1458700.
- Berger M.M., Shenkin A., Schweinlin A., Amrein K., Augsburger M., Biesalski H.K., Bischoff S.C., Casaer M.P., Gundogan K., Lepp H.L., et al. ESPEN micronutrient guideline. Clin. Nutr. 2022;41:1357–1424.
- Biesalski Hans K, Jana T. Micronutrients in the life cycle: requirements and sufficient supply. NFS J. (2018) 11:1–11.
- Salt, About Sodium and Health.
- Ciosek Z., Kot K., Kosik-Bogacka D., Lanocha-Arendarczyk N., Rotter I. The effects of calcium, magnesium, phosphorus, fluoride, and lead on bone tissue. Biomolecules. 2021;11:506.
- Cleveland Clinic. Iron-Deficiency Anemia.
- Doseděl M., Jirkovský E., Macáková K., Krčmová L.K., Javorská L., Pourová J., Mercolini L., Remião F., Nováková L., Mladěnka P., et al. Vitamin C-Sources, Physiological Role, Kinetics, Deficiency, Use, Toxicity, and Determination. Nutrients. 2021;13:615.
- Faba L., Gasa J., Tokach M.D., Varella E., Sola-Oriol D. Effects of supplementing organic microminerals and methionine during the rearing phase of replacement gilts on lameness, growth, and body composition. J. Anim. Sci. 2018;96:3274–3287.
- Fouhy L.E., Mangano K.M., Zhang X., Hughes B.D., Tucker K.L., Noel S.E. Association between a Calcium-to-Magnesium Ratio and Osteoporosis among Puerto Rican Adults. J. Nutr. 2023;153:2642–2650.
- Gibson RS. A historical review of progress in the assessment of dietary zinc intake as an indicator of population zinc status. Adv Nutr. 2012 Nov 1;3(6):772-82.
- Gombart A.F., Pierre A., Maggini S. A review of micronutrients and the immune system-working in harmony to reduce the risk of infection. Nutrients. 2020;12:236.
- Gropper SS, Smith JL, Groff JL. Advanced Nutrition and Human Metabolism. 5th ed. Belmont (CA): Thompson Brooks/Cole; 2009.
- Hosseini S.M., Panahi-Azar A., Sheybani-Arani M., Morovatshoar R., Mirzadeh M., Salimi Asl A., Naghdipour Mirsadeghi M., Khajavi-Mayvan F. Vitamins, minerals and their maternal levels’ role in brain development: An updated literature-review. Clin. Nutr. ESPEN. 2024;63:31–45.
- Lakhal-Littleton S., Robbins P.A. The interplay between iron and oxygen homeostasis with a particular focus on the heart. J. Appl. Physiol. (1985) 2017;123:967–973.
- Lukaski HC. Vitamin and mineral status: effects on physical performance. Nutrition., 20 (2004), pp. 632-644
- Micke O., Vormann J., Kraus A., Kisters K. Serum Magnesium: Time for a Standardised and Evidence-Based Reference Range. Magnes. Res. 2021;34:84–89.
- Mitra S., Paul S., Roy S., Sutradhar H., Bin Emran T., Nainu F., Khandaker M.U., Almalki M., Wilairatana P., Mubarak M.S. Exploring the Immune-Boosting Functions of Vitamins and Minerals as Nutritional Food Bioactive Compounds: A Comprehensive Review. Molecules. 2022;27:555.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Calcium Fact Sheet for Health Professionals.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Copper Fact Sheet for Health Professionals.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Iron Fact Sheet for Health Professionals.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Magnesium Fact Sheet for Health Professionals.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Selenium Fact Sheet for Health Professionals.
- The Nutrition Source. Vitamins and Minerals.
- National Institutes of Health (NIH), Office of Dietary Supplements (ODS). Zinc Fact Sheet for Health Professionals.
- Vitamins and minerals.
- Rippin HL, Hutchinson J, Jewell J, Breda JJ, Cade JE. Adult Nutrient Intakes from Current National Dietary Surveys of European Populations. Nutrients 2017;9(12).
- Rosanoff A., Dai Q., Shapses S.A. Essential nutrient Interactions: Does low or suboptimal magnesium status interact with vitamin D and/or calcium status? Nutr. 2016;7:25–43.
- Skrajnowska D., Bobrowska-Korczak B. Role of Zinc in Immune System and Anti-Cancer Defense Mechanisms. Nutrients. 2019;11:2273.
- The Nutrition Source. Selenium.
- Sustainable Elimination of Iodine Deficiency.
- van Dronkelaar C., van Velzen A., Abdelrazek M., van der Steen A., Weijs P.J., Tieland M. Minerals and Sarcopenia; The Role of Calcium, Iron, Magnesium, Phosphorus, Potassium, Selenium, Sodium, and Zinc on Muscle Mass, Muscle Strength, and Physical Performance in Older Adults: A Systematic Review. J. Am. Med. Dir. Assoc. 2018;19:6–11.e3.
- Vincent JB. New Evidence against Chromium as an Essential Trace Element. J Nutr. 2017 Dec;147(12):2212-2219.
- Weyh C., Krüger K., Peeling P., Castell L. The Role of Minerals in the Optimal Functioning of the Immune System. Nutrients. 2022;14:644.
- Williams MH. Dietary supplements and sports performance: minerals. J Int Soc Sports Nutr., 2 (2005), pp. 43-49
- Yücel K., Gürbüz A.F. Evaluation of calcium/magnesium ratio in patients with type 2 diabetes mellitus. Turk J. Biochem. 2023;48:327–334.



