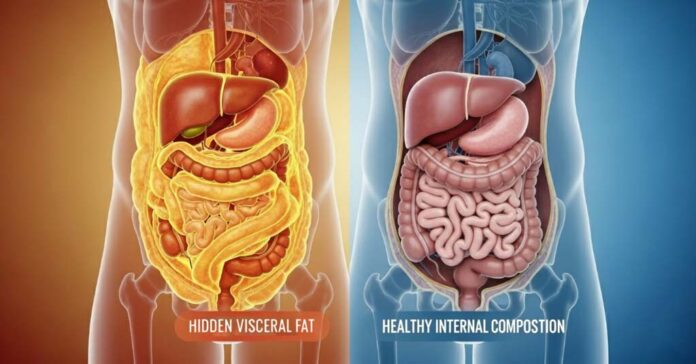
Millions of people with normal weight believe their health is protected. The scales show acceptable numbers. Body mass index calculations fall within recommended ranges.
Medical professionals offer reassurance. Yet research reveals a troubling reality: normal weight provides no immunity against metabolic (energy and biochemical processes in the body) disease when fat accumulates in dangerous locations.
Approximately 30% of individuals classified as normal weight harbour excessive visceral fat (fat packed around internal organs). This hidden adiposity (body fat) drives the same disease processes seen in obviously overweight individuals. Heart disease develops. Diabetes emerges. Blood pressure climbs. The contradiction baffles patients and clinicians alike.
The explanation lies in where fat resides, not how much exists. Someone carrying 15 kg of subcutaneous fat (fat beneath the skin) may show better metabolic health than someone with 8 kg concentrated around their liver and intestines. Total weight reveals nothing about this distribution. BMI captures even less.
Standard health assessments miss this entirely. A person measuring 165 cm and weighing 65 kg has a BMI of 23.9, which is considered a normal weight. Blood pressure reads 118/76 (systolic/diastolic, measuring pressure during and between heartbeats). Cholesterol shows acceptable levels.
Annual check-ups pass without concern. Meanwhile, visceral fat accumulates silently, releasing inflammatory molecules and disrupting insulin function (blood sugar regulation).
This post explores why fat distribution is more significant than total weight for maintaining metabolic health. The data reveals how waist circumference exposes risks that weight-based measures cannot detect. We’ll see why metabolic health depends more on fat location than total quantity, and what this means for people who’ve always fallen within “healthy” weight ranges.

The Body Mass Index Blind Spot
What exactly does BMI measure? Body weight divided by height squared. Nothing more. The calculation treats all tissue identically: muscle, bone, fat, and fluid. A bodybuilder weighing 95 kg at 180 cm registers the same BMI as someone with identical measurements but 30% body fat.
The metric originated from the population studies of 19th-century Belgian mathematician Adolphe Quetelet. He sought statistical patterns, not medical diagnostics. Yet BMI became the default health screening tool globally. Insurance companies adopted it. Government health agencies incorporated it into their guidelines. Clinicians use it automatically.
Research tracking 221,934 people across 17 countries found that BMI failed to predict cardiovascular events in 40% of cases. In contrast, waist circumference was successful in predicting these events. The divergence occurred most dramatically in people classified as normal weight who carried abdominal fat. Their risk matched that of obviously overweight individuals, yet BMI flagged nothing.
Athletes demonstrate BMI’s absurdity clearly. Rugby players frequently have a BMI above 30 (which is technically considered obese). Their body fat percentages range from 12% to 15%. Metabolic health markers show excellence. Meanwhile, sedentary normal weight individuals with BMI of 23 often carry dangerous visceral fat loads. The measurement cannot distinguish between these opposite scenarios.
Why weight-based measures fail:
- Treat muscle and fat identically
- Ignore anatomical distribution entirely
- Provides no insight into metabolic function
- Miss normal-weight obesity completely
Body composition matters infinitely more than total mass. Two people weighing 70 kg may differ dramatically in their health risk depending on whether their adipose tissue is located subcutaneously or viscerally. BMI reveals nothing about this distribution.
The metric also fails to accurately represent ethnic populations. Research shows that Asian individuals develop metabolic dysfunction at BMI levels considered safe for European populations. A Chinese person with a BMI of 24 may carry as much visceral fat as a European person with a BMI of 28. Using universal thresholds misclassifies risk systematically.
Age-related changes expose another limitation. Older adults commonly lose muscle mass while gaining fat. Total weight stays constant. BMI remains unchanged. Yet body composition shifts dramatically towards greater adiposity. Normal weight elderly individuals may harbour substantial visceral fat whilst appearing metabolically healthy by BMI standards. The transformation escapes detection entirely.
Women experience similar invisibility postpartum. Studies following mothers for five years after delivery found that many retained abdominal fat whilst losing lean mass. Overall weight returned to pre-pregnancy levels. BMI looked reassuring. Waist circumference told a different story.
When Normal Weight Hides Dangerous Fat
The phenomenon carries a clinical name: normal-weight obesity. Research defines it as a BMI below 25 with body fat percentage exceeding 30% in women or 23% in men.
Alternatively, being of normal weight by BMI standards, combined with a waist circumference above risk thresholds. Both patterns signal metabolic danger despite reassuring weight measurements.
How common is this condition? Studies using CT scans to measure visceral fat directly found that 20-40% of normal-weight adults carry dangerous levels. The percentage varies by population, age, and activity level. Sedentary individuals show the highest rates. Those with a family history of diabetes face an elevated risk.
Characteristics of Normal-Weight Obesity
Physical presentation appears deceptively healthy. Clothing fits normally. Scales show acceptable numbers. Social comparisons suggest no cause for concern. Yet internal measurements tell a darker story. Visceral fat wraps around the liver. It infiltrates between intestinal loops. The pancreas sits embedded in adipose tissue.
This fat behaves nothing like subcutaneous deposits. It functions as an endocrine organ (hormone-producing tissue), secreting hormones and inflammatory molecules directly into portal circulation (blood flow to the liver).
The liver is constantly bombarded by fatty acids and cytokines (immune signalling proteins). Insulin resistance develops. Blood sugar regulation deteriorates.
Research tracking metabolic markers in individuals of normal weight found striking patterns. Those with elevated waist circumference showed insulin resistance levels matching obviously overweight people.
Their triglyceride levels (blood fats) were high. HDL cholesterol (the protective type) dropped to a low level. Inflammatory markers climbed. The metabolic syndrome (cluster of cardiovascular risk factors) manifested fully despite normal weight.
Cardiovascular outcomes prove equally concerning. A study following 14,828 people for 12.2 years found that normal-weight individuals with central obesity faced higher mortality than those with high BMI but proportional fat distribution. The risk elevation persisted after adjusting for smoking, physical activity, and other factors.
Diabetes development accelerates dramatically in this group. Research examining 76,531 women found that those with normal BMI but elevated waist circumference had 3.9-fold higher diabetes risk compared to normal-weight women with low waist measurements. The risk exceeded that of overweight individuals without central adiposity.
What drives this pattern? Genetics play a role. Some people deposit fat viscerally rather than subcutaneously, regardless of total quantity. Physical inactivity proves critical; muscle loss promotes the accumulation of visceral fat. Dietary factors are particularly important, including processed carbohydrates and industrial fats.
Age and hormones contribute substantially. Postmenopausal women tend to shift towards an android (apple-shaped) fat distribution. Men naturally accumulate visceral fat more readily than premenopausal women. These tendencies intensify without preventive intervention.
The condition affects younger adults increasingly. Studies examining university students found that 12-18% already showed normal-weight obesity patterns. Sedentary lifestyles, poor sleep, and the consumption of ultra-processed foods drive the trend. Early detection allows intervention before metabolic damage becomes irreversible.
What the Research Actually Shows
Evidence from large-scale population studies demonstrates that waist circumference has superior predictive power. The data comes from diverse populations, multiple continents, and decades of follow-up.
The pattern proves consistent: abdominal measurement outperforms weight-based metrics for forecasting disease, particularly in identifying hidden risk amongst normal weight individuals.
One analysis pooled data from 58 prospective studies, including 221,934 participants. Researchers compared BMI against waist circumference for predicting coronary heart disease and stroke. Waist measurement showed stronger associations with both outcomes after adjusting for BMI. Each 5 cm increase in waist circumference raised cardiovascular risk by 13% in men and 17% in women, independent of BMI.
| Study Population | Follow-up Duration | Outcome Measured | Waist Circumference Performance |
|---|---|---|---|
| 359,387 Europeans | 9.7 years | All-cause mortality | 17% increased risk per 5 cm in men, 13% in women |
| 14,828 US adults | 12.2 years | Cardiovascular death | Higher risk in normal BMI + high waist than high BMI alone |
| 76,531 women | 16 years | Type 2 diabetes | 3.9-fold higher risk with normal BMI + elevated waist |
The relationship between waist measurement and metabolic markers proves remarkably linear. Research examining 10,025 adults found that waist circumference correlated more strongly with systolic blood pressure (r=0.34) (pressure during heartbeat), fasting glucose (r=0.28), and triglycerides (r=0.31) (blood fats) than BMI did with any of these markers.
Cancer outcomes show similar patterns. The EPIC study (European Prospective Investigation into Cancer and Nutrition) followed 368,277 participants and found that each 5 cm increase in waist circumference raised colon cancer risk by 13% in men and 9% in women. This association persisted after controlling for BMI, suggesting that abdominal fat drives carcinogenic (cancer-causing) processes independently.
Studies using CT scans to directly measure visceral fat validated waist circumference as a practical surrogate. One investigation comparing anthropometric measurements with CT-quantified visceral adipose tissue found that the waist measurement correlated at r=0.81. BMI managed only r=0.58. The difference proves clinically meaningful.
Research also examined whether combining BMI with waist circumference improved risk prediction beyond the use of either measure alone. Analysis of cardiometabolic risk scores across BMI categories found that waist measurement added substantial predictive value within every BMI group.
The data extends across ethnic populations despite different absolute thresholds. Studies in Asian, Hispanic, African, and European populations all demonstrate the superiority of waist circumference over BMI for predicting metabolic risk. The strength of association varies slightly across populations, but the fundamental pattern remains universally consistent.
Why Visceral Fat Drives Disease Risk
Visceral adipose tissue operates fundamentally differently from subcutaneous deposits. Location determines function.
Fat packed around organs secretes hormones and inflammatory molecules at levels that subcutaneous fat never approaches. This biological activity directly triggers metabolic dysfunction in both overweight and normal weight individuals when visceral accumulation occurs.
The anatomical arrangement creates immediate problems. Visceral fat drains directly into the portal vein (a blood vessel carrying nutrients to the liver), which carries blood to the liver. Every fatty acid, inflammatory cytokine, and hormone released from these deposits flows straight to hepatic tissue. The liver is constantly exposed to pro-inflammatory signals.
This portal drainage pattern proves metabolically catastrophic (severely damaging to the body’s chemistry). When visceral adipocytes (fat cells) release free fatty acids, the liver receives concentrated doses of these acids. Hepatic fat (liver fat) accumulation follows. Insulin signalling becomes impaired. The liver produces excess glucose despite elevated blood sugar. Type 2 diabetes pathophysiology unfolds.
Visceral fat’s metabolic actions:
- Releases fatty acids directly to the liver via the portal vein
- Secretes inflammatory proteins (TNF-alpha, IL-6)
- Produces hormones that disrupt insulin function
- Triggers chronic low-grade inflammation
- Impairs lipid metabolism throughout the body
Inflammatory molecules prove particularly damaging. Visceral fat produces interleukin-6 and tumour necrosis factor-alpha at rates 2-3 times higher than subcutaneous tissue. These cytokines travel systemically, promoting insulin resistance in muscle and liver. They also stimulate C-reactive protein (inflammatory marker) production, driving vascular inflammation.
Research comparing the secretion of adipokines (hormones produced by fat cells) between fat depots revealed dramatic differences. Visceral adipocytes produce less adiponectin (protective hormone) and more leptin (appetite-regulating hormone) than subcutaneous cells. The altered hormone profile promotes the development of metabolic syndrome through multiple pathways.
Lipid metabolism (fat processing) is severely compromised. Visceral fat accumulation associates with elevated triglycerides, reduced HDL cholesterol, and increased small dense LDL (low-density lipoprotein, harmful cholesterol) particles: the exact lipid pattern that maximises cardiovascular risk. This dyslipidemia (abnormal blood fats) can develop even when overall cholesterol levels appear acceptable.
Blood pressure regulation becomes disrupted. Visceral adipose tissue produces angiotensinogen (precursor protein), which converts to angiotensin (blood vessel constrictor) and drives hypertension (high blood pressure). Additionally, insulin resistance itself promotes sodium retention through renal mechanisms. The combination frequently produces blood pressure elevation requiring pharmaceutical intervention.
The cancer connection deserves attention. Visceral obesity promotes carcinogenesis through insulin resistance, chronic inflammation, and sex hormone dysregulation. Research shows that abdominal adiposity increases risk for colon, kidney, liver, and postmenopausal breast cancers independently of total body fat.
What about subcutaneous fat? Studies suggest it may actually provide metabolic protection when visceral deposits remain low. Subcutaneous adipose tissue stores energy relatively inertly. It secretes adiponectin (a protective hormone) at higher rates.
When functioning correctly, it prevents ectopic (abnormally located) fat deposition in the liver and muscle. This explains why individuals with normal weight and a proportional fat distribution exhibit better metabolic health than those with central accumulation. The distinction between depot types proves absolute.

Assessing Your True Risk If You’re Normal Weight
Waist circumference measurement provides a practical solution. The technique requires only a tape measure and correct anatomical landmarks. Unlike CT scans or DEXA (dual-energy X-ray absorptiometry, a body scanning method), anyone can perform the assessment at home. Results classify risk immediately.
The measurement captures abdominal girth at a standardised point. Research established that the midpoint between the lowest rib and the top of the hip bone correlates most strongly with visceral fat measured by imaging. This site proves more reliable than the narrowest visible waist or the umbilicus (belly button), both of which vary substantially between individuals.
Correct measurement technique:
- Locate the lowest rib by feeling downward from the ribcage
- Find the top of the hip bone by placing your hands on your hips
- Mark the exact midpoint between these landmarks
- Wrap tape horizontally at this level
- Ensure the tape remains parallel to the floor completely around the body
- Apply light tension without compressing tissue
- Measure at the end of normal expiration
Timing matters significantly. Measure first thing in the morning after voiding but before eating. A full bladder adds 1-2 cm. Recent food intake temporarily expands the girth by 1-3 cm. Consistent conditions produce reproducible results.
Risk thresholds vary by sex and ethnicity. European men face an increased metabolic risk above 94 cm and a substantial risk above 102 cm. European women show an increased risk above 80 cm, and a substantial risk above 88 cm. These cut-points derive from studies linking waist measurements to disease outcomes.
For individuals with a normal weight according to BMI standards, these thresholds still apply. A woman weighing 60 kg with a waist circumference of 85 cm carries an elevated risk despite an acceptable BMI. Her abdominal fat distribution drives metabolic danger independently of total body mass.
Research following 10,025 adults demonstrates this principle clearly. Within the normal BMI category (18.5-24.9), individuals with waist measurements in the highest tertile (top third of measurements) exhibited 2.7 times higher cardiometabolic risk scores compared to those in the lowest tertile (bottom third of measurements). The effect proved even more pronounced than waist measurement differences across BMI categories.
| Sex | Low Risk | Increased Risk | High Risk |
|---|---|---|---|
| Men | <94 cm | 94–102 cm | >102 cm |
| Women | <80 cm | 80–88 cm | >88 cm |
What should normal weight individuals do if their waist exceeds thresholds? First, verify the measurement using a standardised technique. Repeat on three separate mornings. Use the average value. This eliminates day-to-day biological variation.
Second, obtain comprehensive metabolic screening. Request fasting glucose, HbA1c (3-month average blood sugar), complete lipid panel, and blood pressure assessment. These tests reveal whether visceral adiposity has already triggered metabolic dysfunction.
Third, implement lifestyle modification regardless of current metabolic markers. Visceral fat responds preferentially to exercise and dietary changes. Studies show that moderate interventions can produce a 2-3 cm reduction in waist circumference within 12 weeks, even when overall weight loss remains modest.
For detailed measurement protocols and interactive assessment tools, visit our comprehensive guide to waist circumference measurement.
Sources
- Agbo HA, Zoakah AI, Isichei CO, Sagay AS, Achenbach CJ, Okeahialam BN. Cardiovascular anthropometry: what is best suited for large-scale population screening in Sub-Saharan Africa? Frontiers in Cardiovascular Medicine. 2020;7.
- Armstrong A, Jungbluth Rodriguez K, Sabag A, et al. Effect of aerobic exercise on waist circumference in adults with overweight or obesity: A systematic review and meta‐analysis. Obesity Reviews. 2022;23:e13446.
- Bastien M, Poirier P, Lemieux I, Després JP. Overview of epidemiology and contribution of obesity to cardiovascular disease. Progress in Cardiovascular Diseases. 2014;56(4):369–381.
- Batterham RL, Bedimo RJ, Diaz RS, et al. Cardiometabolic health in people with HIV: expert consensus review. Journal of Antimicrobial Chemotherapy. 2024;79(6):1218–1233.
- Camhi SM, Bray GA, Bouchard C, et al. The relationship of waist circumference and BMI to visceral, subcutaneous, and total body fat: sex and race differences. Obesity. 2011;19(2):402–8.
- Chen L, Zhang J, Zhou N, Weng JY, Bao ZY, Wu LD. Association of different obesity patterns with hypertension in US male adults: a cross-sectional study. Scientific Reports. 2023;13:10551.
- Choudhury KN, Mainuddin AK, Wahiduzzaman M, Islam SM. Serum lipid profile and its association with hypertension in Bangladesh. Vascular Health and Risk Management. 2014;10:327–332.
- Després JP, Moorjani S, Lupien PJ, Tremblay A, Nadeau A, Bouchard C. Regional distribution of body fat, plasma lipoproteins, and cardiovascular disease. Arteriosclerosis. 1990;10(4):497–511.
- Gómez-Ambrosi J, Silva C, Galofré JC, Escalada J, Santos S, Millán D, Vila N, Ibañez P, Gil MJ, Valentí V, Rotellar F, Ramírez B, Salvador J, Frühbeck G. Body mass index classification misses subjects with increased cardiometabolic risk factors related to elevated adiposity. International Journal of Obesity. 2012;36(2):286–294.
- Gunderson EP, Murtaugh MA, Lewis CE, et al. Excess gains in weight and waist circumference associated with childbearing: The Coronary Artery Risk Development in Young Adults Study (CARDIA). International Journal of Obesity and Related Metabolic Disorders. 2004;28(4):525-535.
- Huxley R, Mendis S, Zheleznyakov E, et al. Body mass index, waist circumference and waist:hip ratio as predictors of cardiovascular risk – a review of the literature. European Journal of Clinical Nutrition. 2010;64(1):16-22.
- Janssen I, Katzmarzyk PT, Ross R. Waist circumference and not body mass index explains obesity-related health risk. American Journal of Clinical Nutrition. 2004;79(3):379–384.
- Lear SA, Humphries KH, Kohli S, et al. Visceral adipose tissue accumulation differs according to ethnic background: results of the Multicultural Community Health Assessment Trial (M-CHAT). American Journal of Clinical Nutrition. 2007;86(2):353-359.
- Lear SA, James PT, Ko GT, et al. Appropriateness of waist circumference and waist-to-hip ratio cutoffs for different ethnic groups. European Journal of Clinical Nutrition. 2010;64(1):42-61.
- Manolopoulos KN, Karpe F, Frayn KN. Gluteofemoral body fat as a determinant of metabolic health. International Journal of Obesity. 2010;34:949–959.
- Nazare JA, Smith J, Borel AL, et al. Usefulness of measuring both body mass index and waist circumference for the estimation of visceral adiposity and related cardiometabolic risk profile (from the INSPIRE ME IAA study). American Journal of Cardiology. 2015;115:307–15.
- Neeland IJ, Ross R, Després JP, et al. Visceral and Ectopic Fat, Atherosclerosis, and Cardiometabolic Disease: A Position Statement. Lancet Diabetes & Endocrinology. 2019;7(9):715–725.
- Ren H, Guo Y, Wang D, Kang X, Yuan G. Association of normal-weight central obesity with hypertension: a cross-sectional study from the China health and nutrition survey. BMC Cardiovascular Disorders. 2023;23:120.
- Riley L, Guthold R, Cowan M, Savin S, Bhatti L, Armstrong T, Bonita R. The World Health Organization STEPwise Approach to Noncommunicable Disease Risk-Factor Surveillance: Methods, Challenges, and Opportunities. Am J Public Health. 2016 Jan;106(1):74-8.
- Ross R, Berentzen T, Bradshaw AJ, et al. Does the relationship between waist circumference, morbidity and mortality depend on measurement protocol for waist circumference? Obesity Reviews. 2008;9(4):312-325.
- Sahakyan KR, Somers VK, Rodriguez-Escudero JP, et al. Normal-weight central obesity: implications for total and cardiovascular mortality. Annals of Internal Medicine. 2015;163(11):827–835.
- Seidell JC, Pérusse L, Després JP, Bouchard C. Waist and hip circumferences have independent and opposite effects on cardiovascular disease risk factors: the Quebec Family Study. American Journal of Clinical Nutrition. 2001;74(3):315-321.
- Tchernof A, Despres JP. Pathophysiology of human visceral obesity: an update. Physiological Reviews. 2013;93(1):359–404.
- World Cancer Research Fund/American Institute for Cancer Research Continuous update project. expert report 2018. body fatness and weight gain and the risk of cancer.
- World Health Organization. Waist Circumference and Waist-Hip Ratio: Report of a WHO Expert Consultation. Geneva: World Health Organization. 2008.